Reviewed for clinical accuracy against published literature from the Journal of Prosthetic Dentistry and the International Journal of Oral and Maxillofacial Implants.
Most patients spend weeks researching how much are dental implants before their first consultation. They compare prices, read reviews, and ask about brands. What almost nobody thinks to ask is how the crown sitting on top of their implant is actually held in place. The cement-retained vs screw-retained implants debate has been ongoing in prosthodontic circles for decades, but it almost never reaches the patient. Your ability to get repairs done affordably, and yes, the total cost of your implant over its lifetime.
Most people discover their crown is cemented only if something goes wrong years later and their dentist explains why removing it is complicated. That is not an ideal moment to learn this information. Understanding the difference before treatment begins puts you in a genuinely stronger position at every stage of the process.
This article covers every dimension of the cement-retained vs screw-retained implants comparison that matters to a patient making a real decision in 2026. From clinical risk to cost impact to what U.S. prosthodontists actually recommend today, this is the guide your dentist probably does not have time to walk you through in a standard consultation.
What Cement-Retained vs Screw-Retained Implants Actually Means
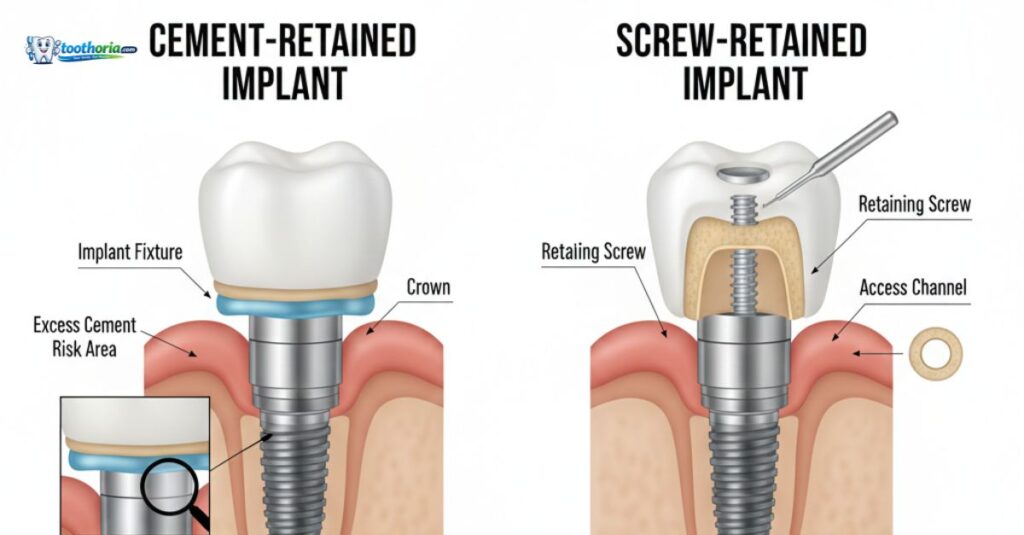
Before comparing the two systems, it helps to understand what each one involves at a practical level, because the terminology alone puts many patients off engaging with the topic at all.
Both systems start identically. A titanium post is surgically placed into your jawbone and left to fuse with the bone over three to six months, a process called osseointegration. The divergence happens entirely at the restoration stage, when the visible crown is attached to the abutment sitting above the gum line.
In a screw-retained system, a small prosthetic screw passes through a channel in the crown and tightens directly into the abutment. That channel, called the screw access hole, is then filled and smoothed with composite material. The crown is mechanically locked in place and can be removed at any future appointment by any qualified dentist who needs access to the implant.
In a cement-retained system, the abutment is fixed to the implant post and the crown is bonded over it using dental cement, in much the same way a crown is placed over a natural prepared tooth. The visible surface of the crown has no hole. It looks completely natural. But it also means the crown cannot be removed without cutting through it, which typically means destroying it entirely and paying for a replacement.
That retrievability gap is the heart of the cement-retained vs screw-retained implants debate, and it has real consequences that compound over the decades you live with your restoration.
How Cement-Retained vs Screw-Retained Implants Affects Your Cost
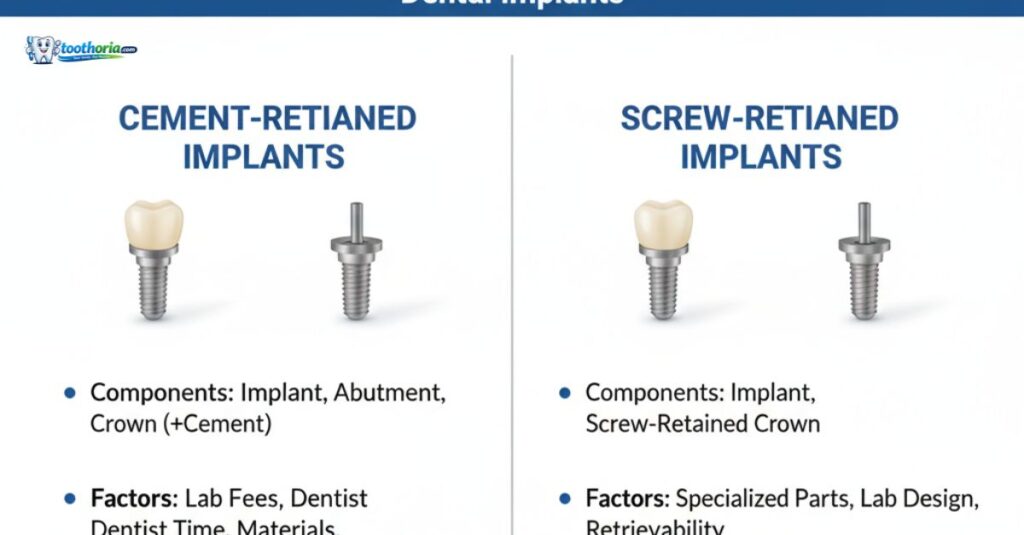
Patients asking how much are dental implants need to understand that the retention system choice has both immediate and long-term cost implications. The surgical phase, which accounts for the largest share of your total investment, is identical for both systems. A titanium implant post costs the same regardless of what holds the crown above it.
The cost difference appears at the abutment and crown fabrication stage. A stock screw-retained abutment typically runs $300 to $600. A custom cement-retained abutment requires additional precision milling to achieve the specific emergence profile the cement system depends on, pushing the cost to $400 to $700. Crown fabrication follows a similar pattern, with cement-retained restorations adding $100 to $300 in laboratory fees due to tighter marginal fit requirements.
The net immediate difference between cement-retained vs screw-retained implants on a single tooth is typically $200 to $500 in total. That modest premium rarely drives the clinical decision, nor should it.
The long-term cost picture is where the comparison gets significantly more interesting. If a screw-retained crown requires attention years down the line, a dentist simply unscrews it, addresses the problem, and replaces it. If a cement-retained crown needs to come off and it cannot be removed intact, the patient pays for a complete crown remake at $1,000 to $2,000 plus any associated treatment cost. Over a 20 to 25 year restoration lifespan, that asymmetry matters more than the initial price difference.
Dr. Carl Misch, one of the most widely cited implant prosthodontists in American dental education and author of the standard U.S. textbook Dental Implant Prosthetics, described retrievability as one of the most undervalued clinical assets in implant restoration planning. His framework, still taught across U.S. dental schools, positions the ability to access and repair a restoration as a core component of its long-term value, not an optional feature.
The Strongest Clinical Case for Screw-Retained Implants
The published evidence over the past fifteen years has moved the professional consensus in U.S. implant dentistry noticeably toward screw-retained systems, and the primary driver is a single, well-documented complication: residual cement.
When a crown is cemented onto an implant abutment inside the mouth, the pressure of seating the crown forces excess cement outward and downward around the margins. A natural tooth has periodontal ligament fibers that create a biological barrier limiting how far this cement can travel. An implant has no such barrier. Research published in the Journal of Periodontology found residual subgingival cement in approximately 81 percent of cement-retained implant cases that later developed peri-implant disease, a destructive inflammatory condition that can ultimately result in implant failure.
Dr. Chandur Wadhwani, a California-based prosthodontist and among the most published U.S. researchers on implant cementation protocols, has documented consistently that even experienced clinicians using careful technique cannot reliably eliminate all subgingival cement. His work, published across multiple issues of the Journal of Prosthetic Dentistry, recommends radio-opaque luting agents specifically so that any residual cement can be identified on post-placement X-rays rather than remaining invisible below the gum line until it causes a problem.
Screw-retained implants eliminate this risk category entirely. There is no cement introduced into the subgingival environment, no contamination pathway, and no need to chase excess material at the margins during seating. For back teeth that will bear heavy biting loads for decades, screw retention also offers structural advantages because the crown relies on mechanical fixation rather than a cement bond to resist the forces of daily function.
When Cement-Retained Implants Are Still the Right Choice
The trend toward screw-retained systems does not make cement retention obsolete. There are specific, well-defined clinical situations where cement-retained implants deliver the better outcome, and understanding them helps patients evaluate their dentist’s recommendation with genuine confidence.
Implant Angulation
The most legitimate indication for cement retention is implant angulation. When an implant has been placed at an angle that would position the screw access hole directly through the visible facial surface of a front tooth, or through a cusp tip in an aesthetically sensitive area, the compromise to the crown design is real. Cement retention in these cases allows the ceramist to work with an uninterrupted crown structure, producing a more natural result in the visible smile zone.
Limited Restorative Space
Cement-retained implants can also be appropriate when the vertical space between the implant platform and the opposing teeth is constrained. Screw-retained systems require a minimum of approximately 6mm of restorative height to accommodate the titanium base and crown thickness. Cement-retained designs can occasionally work within slightly tighter parameters in specific configurations, making them the only viable option in some anatomically restricted cases.
Thin Gingival Biotype
Patients with very thin gum tissue are at aesthetic risk with standard titanium-based screw-retained abutments because the grey metal can cast a visible shadow through the tissue, particularly noticeable in the front of the mouth. In these cases, a zirconia abutment with screw retention or a cement-retained crown on a custom ceramic abutment can produce a significantly more natural gingival appearance. This consideration most often arises in patients exploring how much are dental implants for one front tooth where tissue aesthetics are the primary concern.
It is worth noting that Angulated Screw Channel technology, developed by Nobel Biocare and now available through several implant manufacturers, allows the screw access hole to exit at up to 25 degrees off the implant long axis. This innovation has brought many previously awkward angulation cases within the range where screw retention is viable, meaningfully reducing the number of situations that genuinely require cement retention for aesthetic reasons.
The Screwmentable Option: A Smarter Middle Ground
One solution that most patients never hear about is the screwmentable restoration, a hybrid approach that takes the most valuable features of both systems and combines them into a single design. Understanding this option is particularly relevant when comparing cement-retained vs screw-retained implants for front teeth.
In a screwmentable design, a custom-milled abutment is attached to the implant using a screw, exactly as in a screw-retained system. The crown is then cemented onto that abutment extraorally, meaning outside the mouth in the laboratory or at chairside, before the entire assembly is placed into the patient’s mouth as a single unit.
The clinical advantages are meaningful. The retrieval capability of screw retention is preserved because the entire crown-abutment assembly can be unscrewed from the implant for future access. The cement contamination risk is dramatically reduced because the cementation happens outside the mouth, where excess cement can be thoroughly cleaned under controlled conditions before placement. The aesthetic advantages of cement retention, including a natural emergence profile and the option to avoid a screw access hole on the visible surface, are maintained.
Screwmentable restorations typically cost $3,500 to $5,500 for a single tooth, marginally higher than a purely screw-retained option but representing a risk profile that many experienced U.S. prosthodontists consider superior to either pure system in the right clinical context.
What This Means for Full Mouth and All-on-4 Restorations
For patients researching how much are full mouth dental implants, how much are all on 4 dental implants, or how much are dental implants for the whole mouth, the cement-retained vs screw-retained implants question has a much clearer answer at the arch level.
Full-arch restorations are almost exclusively screw-retained, and the clinical reasoning is compelling. When four to six implants support an entire arch of teeth, the ability to remove, clean, inspect, and eventually replace the prosthetic bridge over the decades it is in service is a genuine maintenance necessity rather than a convenience. Screw-retained full-arch bridges can be removed by a prosthodontist for professional cleaning beneath the prosthesis, inspection of implant tissue health, and material replacement when the prosthetic bridge wears after 15 to 20 years.
A cemented full-arch bridge creates access problems that complicate every aspect of long-term maintenance and dramatically increase the cost of any future repair or replacement. For this reason, patients comparing how much are all on four dental implants across providers should view screw-retained design not as a feature of one clinic but as the clinical standard against which any alternative should be justified.
The Decision Framework Your Dentist Uses
Understanding what factors a prosthodontist evaluates when choosing between cement-retained vs screw-retained implants helps patients engage more productively with the recommendation.
The primary factor is implant position. Where the screw access hole will emerge on the finished crown is determined by the angulation and depth at which the implant was placed in the bone. An ideally positioned anterior implant has its access channel exiting through the cingulum, the back of the crown, completely invisible from the front. An ideally positioned posterior implant has the channel emerging through the central groove of the chewing surface, equally inconspicuous. When those ideal positions are achieved through careful treatment planning, screw retention is almost always the preferred clinical choice.
The secondary factor is restorative space measured from the implant platform to the opposing dentition. Cement-retained restorations require approximately 7 to 8mm of interarch space to accommodate proper abutment height and crown material thickness. Screw-retained restorations can function in as little as 6mm because the titanium base is more compact. In limited-space cases, this distinction can actually favor screw retention.
The third factor is tissue thickness and biotype, which determines whether the abutment material will affect the visible color of the gum around the restoration. This consideration most directly affects patients asking how much are dental implants for one tooth in the visible front smile zone.
Frequently Asked Questions
Which is better, cement-retained or screw-retained implants?
Screw-retained is generally preferred today by most U.S. prosthodontists, primarily because it eliminates residual cement risk and allows future retrieval without destroying the crown.
Do cement-retained implants cost more than screw-retained?
Marginally, typically $200 to $500 more per tooth due to custom abutment fabrication and tighter lab requirements. Not enough to be the deciding factor.
What happens when a cement-retained crown fails?
It usually cannot be removed intact. If the abutment screw loosens beneath it, the crown must typically be cut off and remade at full replacement cost.
Is residual cement actually dangerous?
Yes. Published research links residual subgingival cement to peri-implant disease in a high percentage of affected cases. It is one of the most documented biological risk factors in implant dentistry.
What is a screwmentable implant?
A hybrid system where a screwed abutment is used but the crown is cemented extraorally before placement, preserving retrievability while reducing cement contamination risk. Worth asking about for front teeth.
Conclusion
The cement-retained vs screw-retained implants debate does not have a universal winner because the right answer genuinely depends on the specific clinical situation, implant position, available space, tissue type, and the patient’s long-term maintenance needs. What the evidence does make clear is that screw retention has become the professional default in U.S. implant dentistry for well-documented reasons, and cement retention should be chosen only when a specific clinical indication makes it the better option, not simply because it is familiar or technically simpler for the provider.
The most powerful thing a patient can do before committing to any implant restoration is ask directly: are you using cement-retained or screw-retained, and why? Ask whether angulated screw channel technology or a screwmentable hybrid was evaluated. Ask what the retrieval plan looks like if a problem develops in year ten. Those questions protect your investment far more effectively than negotiating the upfront cost alone. For the complete picture on how much are dental implants across every scenario, from how much are mini dental implants to how much are full mouth dental implants, visit our main dental implant cost guide where every option is covered in full detail.