If you’ve ever needed to visit an oral surgeon, you probably have questions about what’s involved. Maybe you’re facing your first procedure and feel nervous. Or perhaps you’re trying to understand what different surgical options mean for your smile and health.
The good news? Most common types of oral surgery are routine procedures that millions of people undergo successfully each year. Understanding what to expect before, during, and after surgery can ease anxiety and help you prepare properly.
This guide covers the seven most common oral surgery procedures, how they work, realistic recovery timelines, and what you can do to support your healing. For a comprehensive overview of what oral surgery is and when it’s necessary, start with that foundational understanding before diving into specific procedures.
What Is Oral Surgery?
Oral surgery, also known as oral and maxillofacial surgery, refers to any surgical procedure performed on your teeth, gums, jaw, or mouth. These procedures are typically performed by oral surgeons, dentists with specialized training beyond general dental school.
Unlike routine dental cleanings or fillings, oral surgery requires a level of expertise and specialized equipment. Oral surgeons complete at least four additional years of specialized training after dental school. This training covers surgical techniques, anesthesia management, bone grafting, and complex tooth removal.
You might need oral surgery for several reasons. Some procedures save teeth that otherwise would be lost. Others replace missing teeth or correct jaw problems that affect your ability to chew, speak, or breathe properly. Some surgeries are purely cosmetic, while others address serious health concerns.
The common types of oral surgery include everything from simple tooth extractions to complex jaw realignment. Each procedure has its own recovery timeline and aftercare requirements.
Understanding Your Surgical Options
Before diving into specific procedures, it helps to understand what separates different surgical approaches. Some oral surgeries are straightforward and take 15 to 30 minutes. Others are complex and might require several hours or even multiple visits.
Complexity affects three things: how long the procedure takes, how much discomfort you experience afterward, and how long complete healing requires. A simple tooth extraction might involve just local anesthesia and basic removal. A surgical extraction of an impacted tooth requires a small incision, bone removal, and careful technique.
Your surgeon will explain which category your specific situation falls into. They’ll also discuss anesthesia options, which typically include local numbing, IV sedation, or general anesthesia depending on the procedure’s complexity and your comfort level.
Procedure #1: Tooth Extraction (Simple and Surgical)
Tooth extraction is the most common oral surgery procedure. Millions of teeth are extracted each year for various reasons. Sometimes a tooth can be removed with basic instruments. Other times, surgical technique becomes necessary.
When Tooth Extraction Becomes Necessary
You might need a tooth extracted if decay has destroyed most of the tooth structure. Severe infection or abscess can also require extraction if root canal treatment isn’t possible or hasn’t worked. Advanced gum disease sometimes forces extraction when a tooth becomes too loose to save.
Orthodontic treatment might require extraction to create space for teeth alignment. A tooth that develops a serious crack or fracture below the gum line often can’t be salvaged. Teeth that are impacted or stuck under the gum and causing problems also need removal.
How Simple Extraction Works
During a simple extraction, your dentist first numbs the area completely with local anesthesia. Once you’re comfortable, they gently rock the tooth back and forth using specialized instruments called elevators. These loosen the tooth’s attachment to the bone and ligaments holding it in place.
Once loosened enough, the dentist uses forceps to lift the tooth from its socket. The socket is then cleaned to remove any debris. Gauze is placed to stop bleeding. The whole process usually takes 15 to 30 minutes.
Understanding Surgical Extraction
A surgical extraction becomes necessary when the tooth is trapped beneath bone or gum tissue. This might happen with deeply impacted teeth or those with curved or fragile roots.
The surgeon makes a small incision in the gum to access the tooth. Sometimes bone around the tooth needs to be carefully removed to access it properly. The tooth might be divided into smaller sections for easier removal. Each piece is then carefully lifted away.
Once the tooth is out, the area is cleaned thoroughly. Sometimes bone grafting material is placed in the socket to preserve the bone. This is especially important if you’re planning a dental implant later. The area is closed with sutures that usually dissolve on their own within one to two weeks.
Extraction Recovery Timeline
The first 24 hours are critical. Swelling and discomfort peak during this time. You’ll bite on gauze to control bleeding, which should stop within an hour or two. Light bleeding might continue for several hours, which is normal.
By day two or three, swelling reaches its maximum. This looks worse than it feels. You might look significantly puffy around the jaw and cheek. Ice packs during the first 24 hours help minimize this. After that, heat feels better.
Most people return to light activities by day three to five. Complete healing at the surface takes about two weeks. The bone filling in the socket completely takes three to six months.
Aftercare for Extractions
Keep your head elevated for the first few nights to reduce swelling and bleeding. Apply ice for 15 to 20 minutes at a time during the first day. Sleep with an extra pillow for support.
Stick to soft foods like yogurt, mashed potatoes, and smoothies for the first week. What you eat after tooth extraction matters greatly for your healing. Avoid using straws, which create suction that can dislodge the blood clot and cause a painful condition called dry socket.
Know what to avoid after tooth extraction to prevent complications. Don’t rinse, spit forcefully, or smoke for at least a week. Smoking dramatically increases your risk of complications and slows healing. Gentle salt water rinses starting on day two help keep the area clean.
Pain is usually manageable with over-the-counter pain relievers. If pain worsens after several days, contact your surgeon immediately. This might indicate an infection or dry socket, which requires special home remedies and professional care.
Procedure #2: Wisdom Teeth Removal
Wisdom teeth are your third molars, which typically emerge between ages 17 and 25. Many people develop problems with these teeth, making removal one of the most common oral surgery procedures.
Why Wisdom Teeth Need Removal
Your jaw might not have space for four additional molars. When teeth emerge in this crowded space, they can damage neighboring teeth or grow at painful angles. Some wisdom teeth emerge partially, creating a pocket where bacteria accumulate and cause infections.
Impacted teeth trapped below the gum line can cause swelling, pain, and infection even without ever fully emerging. Cysts or tumors sometimes develop around impacted wisdom teeth. Some people get them removed preventively to avoid problems later.
The Wisdom Tooth Removal Process
Your surgeon takes X-rays first to plan the best approach. The procedure begins with anesthesia, typically IV sedation that lets you relax and forget most of the experience. A local numbing injection ensures you feel no pain.
The surgeon makes an incision in the gum if needed. If bone blocks the tooth, it’s carefully removed. The tooth might be divided into sections for easier removal. Each piece is gently lifted away using elevators.
The socket is then cleaned and inspected for any remaining tooth fragments. Some surgeons place bone grafting material to preserve the socket. The area is closed with sutures.
Recovery From Wisdom Tooth Surgery
Expect more swelling and discomfort than simple extractions because more surgical work is involved. The first 48 hours are the most uncomfortable. Swelling peaks around day two or three, then improves quickly.
Most people feel significantly better by day five to seven and can return to normal activities. Some tenderness might persist for several more days. Unlike some surgeries, wisdom tooth removal typically allows faster return to normal eating and activity.
Jaw stiffness sometimes develops, limiting how wide you can open your mouth. This resolves within one to two weeks. Mild bruising occasionally appears and fades over several days.
Managing Wisdom Tooth Recovery
Use ice aggressively the first day. Alternate 20 minutes on and off to minimize swelling. Starting day two, switching to warm compresses feels better.
Pain medication is important the first few days. Your surgeon will provide prescriptions if needed. Over-the-counter pain relievers might not be enough for the first 48 hours.
Eat soft, cold foods the first week. Smoothies, pudding, ice cream, and yogurt are ideal. Avoid hot foods, which increase swelling. No straws, smoking, or vigorous rinsing for at least one week.
Procedure #3: Dental Implants
Dental implants replace missing teeth with a permanent solution that looks, feels, and functions like natural teeth. Unlike removable dentures or traditional bridges, implants are anchored directly to your jawbone.
How Implants Restore Your Smile
An implant consists of three parts. The implant itself is a titanium post surgically inserted into your jawbone. Over several months, bone grows around this post in a process called osseointegration. This creates a solid foundation.
An abutment is then placed on top of the implant. This connector piece protrudes above the gum line. Finally, a custom crown is placed on the abutment, creating a tooth that looks like your natural teeth.
For single tooth replacement, implants offer superior longevity compared to traditional bridges. If you’re considering tooth replacement options, understanding how much dental implants cost in 2026 helps with financial planning. You might also compare implants with dental bridge costs and options to determine which solution fits your needs and budget.
When You Need Bone Grafting First
Your jawbone needs adequate volume and density to support an implant. If you’ve worn dentures for years or had severe gum disease, bone might have resorbed away.
In these cases, bone grafting comes first. Your surgeon adds bone material to build up the jaw. This process takes three to six months before implant placement. We’ll cover bone grafting in detail shortly.
The Implant Placement Process
Before surgery, your surgeon takes 3D imaging to plan optimal implant positioning. This ensures the implant angles properly and provides maximum support.
The procedure begins with anesthesia, typically IV sedation combined with local numbing. The surgeon makes an incision in the gum to access the bone. Using specialized drill bits of increasing sizes, a precise hole is created in the bone.
The titanium implant is carefully threaded into place. It’s torqued to a specific pressure to ensure stability without damaging the bone. The gum is then closed over the implant with sutures that dissolve over one to two weeks.
For the next three to six months, you must avoid putting pressure on the implant while osseointegration occurs. You’ll stick to soft foods and avoid chewing on that side. If you’re concerned about compatibility with medical procedures, dental implants are safe for MRI imaging when properly placed.
Once bone has fully integrated, a second minor procedure exposes the implant. A healing cap is placed, and your gums heal around it over one to two weeks. Then your dentist makes the crown.
Recovery and Expectations
Initial recovery takes one to two weeks. Expect swelling, discomfort, and mild bleeding. Ice helps the first 24 hours. Pain medication eases discomfort.
The hardest part is waiting for osseointegration. You can return to normal activities within a week, but you must protect the implant site from pressure. No chewing on that side, even soft foods, for several months.
Your surgeon will schedule follow-up visits to monitor healing and take X-rays confirming osseointegration. Once that’s complete, implant crown placement restores your normal eating and speaking ability.
Procedure #4: Bone Grafting and Ridge Augmentation
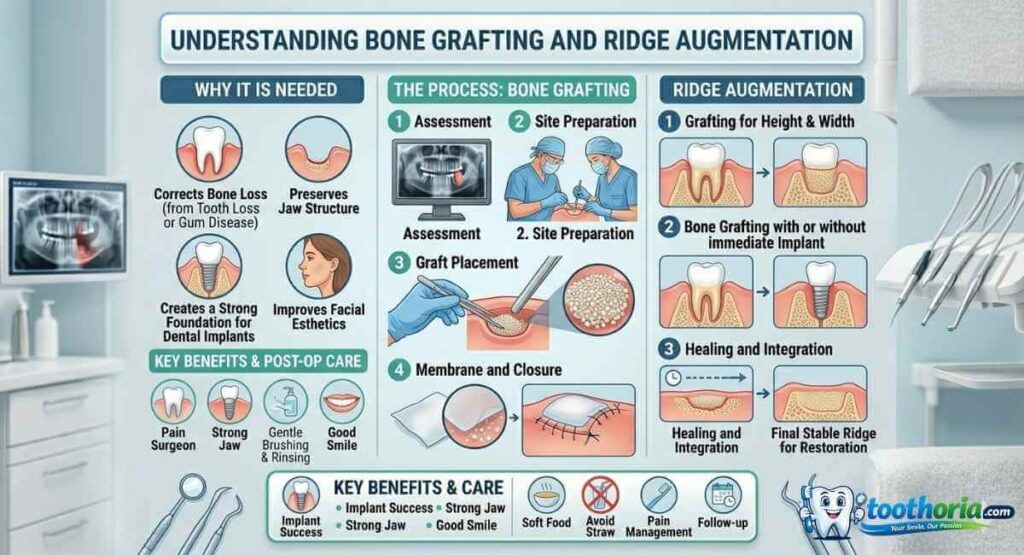
Bone grafting rebuilds jawbone that has been lost due to gum disease, missing teeth, or trauma. This procedure is essential for many implant patients and helps stabilize teeth affected by advanced periodontal disease.
Understanding Bone Loss
When teeth are missing, the bone supporting them slowly resorbs, or shrinks away. This process accelerates over time. People with untreated gum disease experience significant bone loss. Trauma, infection, or cancer treatment can also destroy jaw bone.
Bone loss creates several problems. Remaining teeth become loose and less stable. Facial appearance changes, sometimes dramatically. Implants can’t be placed without sufficient bone.
How Bone Grafting Works
Your surgeon evaluates the extent of bone loss with imaging. They determine how much bone material is needed and where it should be placed.
The graft material can come from several sources. Autogenous bone, taken from another part of your jaw or body, offers excellent results but requires a second surgical site. Allograft material comes from donor bone. Xenograft uses bone from animal sources. Synthetic bone substitutes are also available.
During the procedure, the surgeon makes a small incision to access the bone. The graft material is shaped and positioned carefully. A barrier membrane sometimes is placed to prevent gum tissue from growing into the graft site.
The area is then closed with sutures. Over the next four to six months, your body gradually replaces the graft material with your own bone. This integration process is critical and requires you to protect the graft site.
Bone Graft Recovery and Timeline
The first week involves significant discomfort, swelling, and sensitivity. Ice helps initially. Pain medication eases discomfort, which is usually manageable with over-the-counter options.
Weeks two through six show gradual improvement. Swelling subsides. You transition to a more normal diet, though you must still avoid chewing hard or sticky foods near the graft site.
For the next several months, you see no obvious changes. Bone is integrating invisibly beneath your gum line. Avoid smoking, vigorous exercise, and anything that might disturb the graft.
At three months, your surgeon might take new X-rays to confirm integration is progressing. By six months, bone is usually ready for implant placement if that’s your plan.
Protecting Your Graft
This is critical. Don’t chew near the graft site for at least two weeks. Soft diet for three to four weeks minimizes stress.
Avoid smoking entirely. Nicotine constricts blood vessels and dramatically impairs healing. Some studies suggest smokers have twice the graft failure rate of non-smokers.
Sleep elevated for the first few nights. Maintain excellent oral hygiene without disturbing the graft. Gentle water rinses are better than vigorous rinsing in the early weeks.
Periodontal Surgery
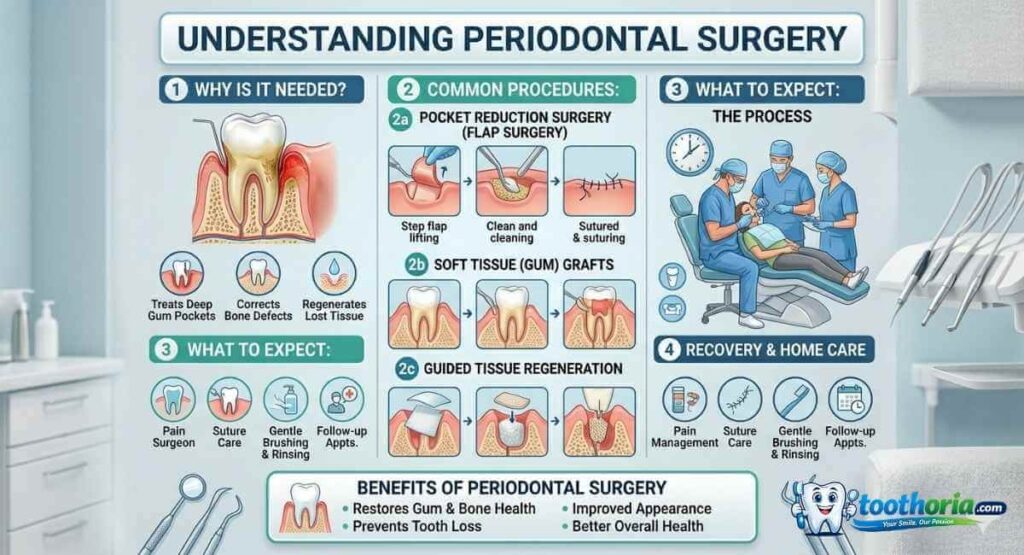
Periodontal surgery treats advanced gum disease when conservative treatments haven’t been sufficient. These procedures can save teeth that otherwise would be lost to bone loss and infection.
Sometimes, even before reaching the need for surgery, you might notice loose teeth in adults developing from gum disease. Early intervention at this stage can prevent the need for surgical treatment. Understanding the stages a loose tooth progresses through helps you seek care before bone loss becomes severe.
When Gum Disease Requires Surgery
Early gum disease might respond to thorough cleaning and improved home care. But moderate to advanced periodontitis, with deep pockets and significant bone loss, often needs surgical intervention.
Your periodontist might recommend surgery if pockets deeper than five millimeters remain after non-surgical treatment. Significant bone loss visible on X-rays often requires surgery. Teeth becoming loose from bone loss need surgical support.
Understanding the stages of gum disease and available treatment options helps you recognize when surgery might be necessary. Early detection and intervention can prevent advanced disease requiring surgical treatment.
Flap Surgery and Bone Contouring
In flap surgery, the periodontist makes precise incisions along the gum line. The gum is gently folded back like a flap to expose the bone beneath.
With better access, the surgeon removes disease-causing bacteria and tartar from surfaces that regular cleaning can’t reach. Damaged bone is carefully reshaped to eliminate deep pockets. Sometimes bone grafting material is added to regenerate bone loss.
The gum flap is then repositioned and sutured. The new pocket depth is shallower, making the area easier for you to clean at home.
Graft Surgery for Recession
Severe gum recession exposes root surfaces, causing sensitivity and aesthetic concerns. Graft surgery restores lost gum tissue.
If you’re experiencing gum recession and want to understand your treatment options, surgical grafting offers a permanent solution. The surgeon takes a graft from your palate or uses donor graft material. This is carefully sutured over the exposed root. The graft’s blood supply gradually establishes, and the graft becomes permanent living tissue.
For managing sensitivity from recession between procedures, using the right toothpaste specifically formulated for gum recession can provide relief.
Recovery From Periodontal Surgery
Initial recovery takes one to two weeks. The area feels tender and sensitive. Some bleeding might occur, which is normal.
Starting day two or three, gentle salt water rinses help keep the area clean. Avoid brushing the surgical site for at least two weeks. Use prescribed antimicrobial rinse instead.
Pain is usually mild to moderate and manageable with over-the-counter pain relievers. Swelling subsides within one week. Most people return to work after a few days.
The real healing happens over weeks and months. Bone regenerates slowly. Graft tissue matures and becomes stronger over two to three months.
Procedure #6: Endodontic Surgery
Endodontic surgery treats tooth infections that root canal therapy alone hasn’t resolved. These procedures save teeth that might otherwise be extracted.
When Endodontic Surgery Becomes Necessary
Root canal therapy successfully saves most infected teeth. But sometimes the infection persists despite quality root canal treatment. This might happen because calcium deposits blocked access to the entire canal system. A crack below the gum line might harbor infection.
In these cases, endodontic surgery, usually a procedure called apicoectomy, removes the infected root tip directly.
The Apicoectomy Procedure
The endodontist makes a small incision in the gum above the tooth’s root tip. Bone is carefully removed to access the root apex.
The inflamed tissue surrounding the root tip is removed. About three millimeters of the root tip itself is also removed. Under magnification, the surgeon inspects the root to ensure all infected tissue is eliminated.
A small filling is then placed in the root tip using biocompatible material. The bone and gum are sutured closed.
Recovery From Endodontic Surgery
Recovery is faster than many surgical procedures. The first day involves mild discomfort, some swelling, and possibly slight bleeding.
Most people feel significantly better by day two. Pain is usually manageable with over-the-counter pain relievers. Swelling subsides within a week.
You should avoid chewing near the surgical site for one week. A soft diet during initial recovery helps. Most people return to normal activities within a few days.
Complete healing takes several months as bone regenerates around the treated tooth. Your endodontist will monitor healing with X-rays at follow-up appointments.
Procedure #7: Corrective Jaw Surgery
Corrective jaw surgery, called orthognathic surgery, realigns your jaw to correct bite problems and improve facial structure. This is the most complex procedure among common types of oral surgery.
Why Jaw Surgery Becomes Necessary
Severe bite problems that can’t be corrected with braces alone might require jaw surgery. An underbite where your lower jaw extends too far forward affects function and appearance. An overbite where your upper jaw is too prominent creates similar issues.
Open bite, where front teeth don’t touch when your mouth is closed, prevents proper chewing. An asymmetrical jaw where one side is significantly larger creates functional and aesthetic problems.
Sleep apnea caused by jaw position might improve with surgery. TMJ problems related to jaw misalignment sometimes require surgical correction.
Before the Surgery: Orthodontic Preparation
Most jaw surgery requires 12 to 24 months of braces before surgery. These aren’t cosmetic braces for straightening teeth. Pre-surgical braces align your teeth to the corrected jaw position you’ll have after surgery.
Understanding the cost of orthodontic braces and different types available helps you budget for this pre-surgical phase. Your surgeon and orthodontist work together to plan the surgery. Computer simulations show what your face will look like afterward. 3D imaging helps plan exact surgical positioning.
The Surgery Process
Jaw surgery is performed under general anesthesia, usually in a hospital setting. The surgeon makes incisions inside your mouth, avoiding visible facial scars.
For lower jaw surgery, incisions are made below the teeth. The jawbone is cut at precise locations and moved to the correct position. Titanium plates and screws secure it permanently.
For upper jaw surgery, similar techniques reposition your upper jaw. Many patients need both upper and lower jaw adjusted, called bimaxillary surgery.
The entire procedure might take two to four hours, depending on complexity.
Recovery From Jaw Surgery
This is the longest recovery of all common types of oral surgery. The first week involves significant swelling, discomfort, and bruising. Many surgeons recommend hospital stay or recovery facility observation for the first night.
Your jaw might be wired shut initially, requiring a liquid diet. Some surgeons avoid wiring now, allowing you to eat soft foods immediately.
The first week is the most challenging. Swelling peaks around day two or three. Strong pain medication helps manage discomfort. You’ll need to take time off work or school.
By week two, you can eat soft foods without chewing effort. Swelling gradually improves over the next several weeks. Most people return to light activities by week three to four.
Complete healing takes six to twelve months. Your bite continues improving as bone fully heals. Braces remain for several months after surgery for final bite refinement.
General Recovery Principles Across All Oral Surgery
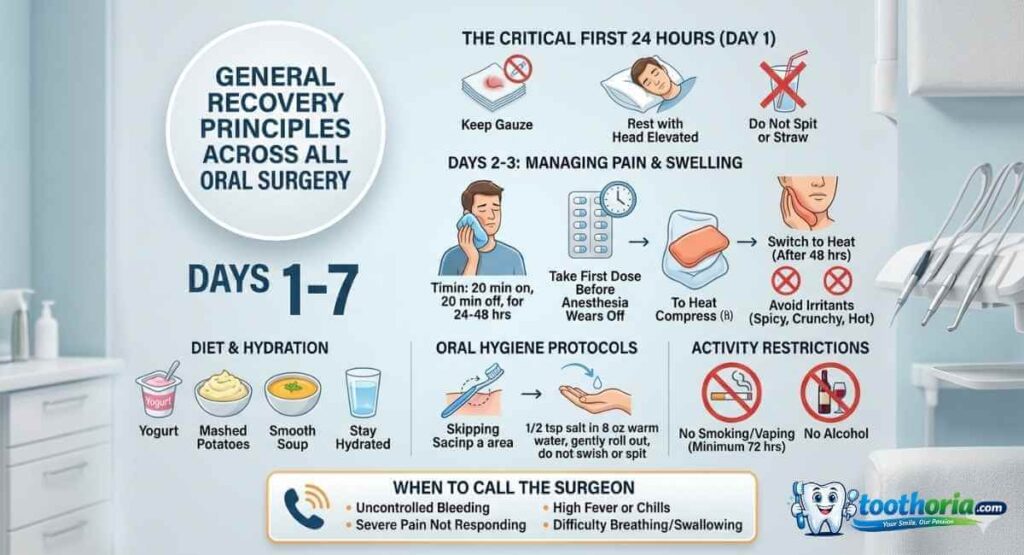
Regardless of your specific procedure, some recovery principles apply broadly.
Maintaining proper dental hygiene with the right food choices and care techniques during your recovery prevents complications and promotes faster healing.
The First 24 Hours Are Critical
Immediately after surgery, follow your surgeon’s instructions precisely. Bite on gauze if directed. Apply ice as instructed. Avoid rinsing, spitting, and other activities that might disturb the surgical site.
Rest completely the first day. Your body is healing and needs energy for recovery. Mild bleeding is normal. Continued heavy bleeding should be reported to your surgeon.
Managing Swelling and Pain
Swelling typically peaks around day two or three after surgery, then improves. Ice during the first 24 hours significantly reduces swelling. After 24 hours, most surgeons recommend switching to heat if you prefer.
Pain is usually worst the first few days. Your surgeon will provide pain medication if needed. Don’t tough it out. Proper pain control helps you rest and heal better.
Sleep elevated with an extra pillow for the first few nights. Elevation reduces swelling and promotes healing.
Diet and Nutrition Matter
Avoid hard, crunchy, hot, and spicy foods initially. These irritate the surgical site and can cause complications. Soft foods provide adequate nutrition while protecting your healing tissues.
Stay hydrated. Your body needs fluids for healing. Avoid alcohol during the first week, as it impairs healing and interacts with pain medications.
When to Call Your Surgeon
Contact your surgeon immediately if you experience fever over 101 degrees Fahrenheit. Excessive bleeding that doesn’t stop after 30 minutes of pressure needs attention.
Severe pain that worsens after several days, rather than improving, might indicate infection or other complications. If you suspect a gum infection, knowing the best antibiotics for treatment helps you get prompt care. Swelling that worsens after the first three days should be evaluated.
Difficulty swallowing or breathing requires emergency attention. Allergic reactions like rash or difficulty breathing need immediate care.
Frequently Asked Questions About Oral Surgery
Will I be asleep during oral surgery?
It depends on the procedure and your preference. Simple extractions might use just local numbing. Wisdom teeth removal typically uses IV sedation that makes you relaxed and forgetful. Complex procedures like jaw surgery use general anesthesia. Your surgeon will discuss options beforehand.
How painful is oral surgery?
You should feel no pain during surgery due to anesthesia. You might feel pressure, vibration, or hear sounds, but not pain. After surgery, discomfort varies by procedure. Simple extractions cause mild discomfort. Jaw surgery causes more significant pain that requires prescription medication.
How long until I can eat normally?
This varies dramatically. After simple extraction, you can eat soft foods immediately and resume normal diet within one to two weeks. After implant placement, you must protect the site for several months. After jaw surgery, soft diet continues for weeks to months.
Can I go to work after oral surgery?
For simple procedures, many people return to desk work the next day. Procedures involving more swelling, like wisdom teeth removal or bone grafting, might require a few days off. Jaw surgery requires two to four weeks away from work typically.
What’s dry socket and how do I prevent it?
Dry socket occurs when the blood clot protecting the extraction socket dislodges. Bacteria or air exposure causes severe pain. Prevent it by avoiding straws, spitting forcefully, smoking, and aggressive rinsing for at least one week.
Does smoking really affect healing?
Yes, significantly. Nicotine constricts blood vessels, reducing healing blood flow. Smoking increases infection risk and complications. Smokers have higher failure rates for procedures like implants and grafts. Avoid smoking for at least one week, ideally longer.
Conclusion
Common types of oral surgery range from straightforward procedures most people handle easily to complex surgeries requiring significant recovery time. Understanding your specific procedure, what to expect during recovery, and how to support your healing gives you the confidence to move forward.
Your surgeon is your best resource for personalized information about your situation. Don’t hesitate to ask questions. Understanding your treatment plan helps you prepare properly and achieve the best outcome.
Most oral surgery complications are preventable through careful adherence to aftercare instructions. Take it seriously. The effort you invest in recovery the first week pays enormous dividends in healing and results.
If you’re facing an oral surgery procedure, you’ve got this. Millions of people successfully undergo these procedures each year and return to normal life quickly. With proper preparation and care, you will too.