You’re sitting in the dentist’s chair. Your dentist takes one look at your X-ray, leans back, and says, “I think you need to see an oral surgeon.” Your stomach drops. You weren’t expecting that.
But don’t panic. Oral surgery sounds scary, but millions of people go through it every year and most of them walk out feeling a whole lot better than they did walking in.
So what exactly is oral surgery? Who performs it? And do you actually need it? This guide covers everything you need to know, in plain English.
What Is Oral Surgery?
Oral surgery refers to any surgical procedure performed in or around your mouth. That includes your teeth, gums, jawbone, and the surrounding facial structures.
It’s a broad term. A simple tooth pulling counts as oral surgery. So does placing a dental implant, reshaping your jaw, or removing a cyst. The common thread is this: these procedures go beyond what a regular dentist handles in a routine appointment.
Oral surgery falls under a field called oral and maxillofacial surgery. “Maxillofacial” is just a fancy way of saying the jaw and face area. The American Dental Association (ADA) recognizes it as one of nine official dental specialties. That tells you how serious and established this field really is.
What Does an Oral Surgeon Do?
An oral surgeon isn’t just a dentist with extra tools. The training is significantly more involved.
After completing dental school, an oral surgeon goes through four to six years of hospital-based surgical training. During that time, they work alongside medical doctors in departments like general surgery, internal medicine, anesthesiology, and emergency medicine. Some even earn a medical degree on top of their dental degree.
This level of training allows them to handle cases that are simply too complex for a general dentist.
How Is an Oral Surgeon Different From Other Specialists?
People often mix up oral surgeons with other dental specialists. Here’s a quick breakdown:
- A periodontist focuses on gum disease and the structures that support your teeth.
- An endodontist specializes in root canals and the inside of your teeth.
- An oral surgeon handles surgical cases involving teeth, bone, jaws, and the broader facial region.
In many situations, your dentist will treat you just fine. But when things get complicated, whether that’s an impacted tooth, bone loss, or a jaw problem, they’ll refer you to an oral surgeon.
Common Types of Oral Surgery
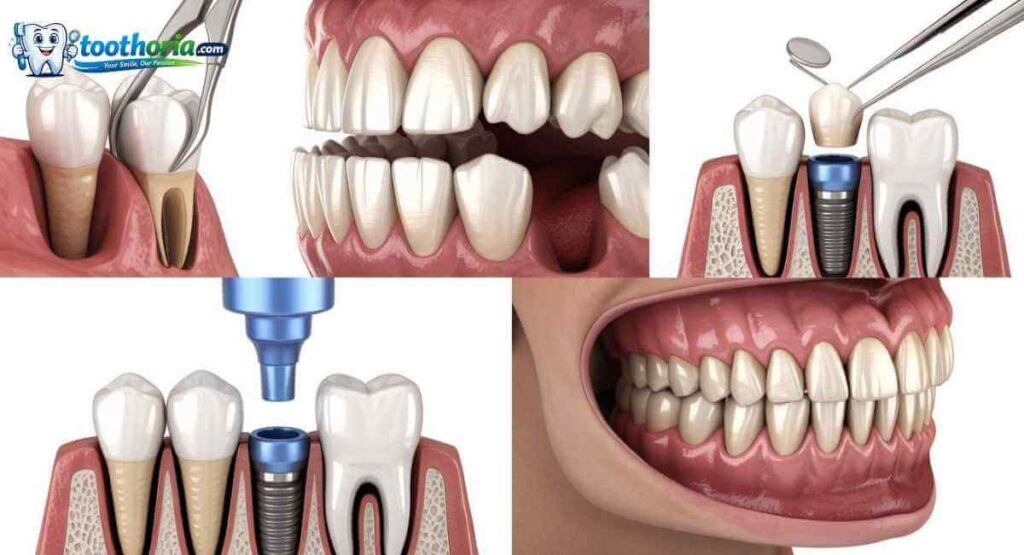
Oral surgery covers a wider range of procedures than most people realize. Here are the most common ones.
1. Tooth Extraction
This is the most common type of oral surgery. Sometimes, a tooth is too damaged, decayed, or crowded to save. When that happens, it has to come out.
Simple extractions are straightforward. Surgical extractions are needed when a tooth is broken below the gum line or hasn’t fully come in yet. Your dentist can handle simple ones, but surgical extractions are done by an oral surgeon.
2. Wisdom Tooth Removal
Your wisdom teeth are your third molars, the last set of teeth to grow in, usually in your late teens or early twenties. Because most people’s mouths don’t have room for them, they often grow in at awkward angles or get stuck beneath the gum. This is called impaction.
Impacted wisdom teeth can cause pain, swelling, infection, and damage to nearby teeth. That’s why removing them early is often the smartest move, even before they cause obvious problems.
3. Dental Implants
If you’ve lost a tooth, a dental implant is the closest thing to getting your natural tooth back.
An oral surgeon places a small titanium post directly into your jawbone. Over the following months, the bone fuses to the post in a process called osseointegration. Once that’s done, a crown is attached on top. The result looks and functions almost exactly like a real tooth.
Dental implants have a success rate of over 95%, which makes them one of the most reliable procedures in modern dentistry.
4. Dental Bone Graft
When you lose a tooth, the jawbone beneath it slowly starts to shrink. There’s nothing stimulating it anymore, so the body stops maintaining it.
A bone graft adds volume back to your jaw. It’s often needed before placing a dental implant, so the post has enough solid bone to anchor into. Grafting material can come from your own body, a donor, or a synthetic source.
5. Corrective Jaw Surgery (Orthognathic Surgery)
Sometimes the upper and lower jaw don’t line up the way they should. This can affect how you chew, how you breathe, and even how you speak.
Corrective jaw surgery repositions one or both jaws to fix the alignment. People with severe overbites, underbites, or asymmetrical jaw growth often benefit from this procedure. Recovery takes time, but the improvement in daily function can be dramatic.
6. Gum Graft Surgery
When your gums recede too far, they expose the roots of your teeth. Exposed roots are sensitive. They’re also more vulnerable to decay and infection.
A gum graft takes tissue, usually from the roof of your mouth, and uses it to cover the exposed area. It stops further recession and reduces sensitivity. If you’ve noticed your teeth looking “longer” than they used to, that’s a sign your gums may be pulling back.
7. Sleep Apnea Surgery
For people with severe obstructive sleep apnea who can’t tolerate a CPAP machine, surgery is sometimes an option.
Certain procedures can reposition the jaw or remove tissue from the throat and palate to open up the airway. An oral and maxillofacial surgeon with specialized training performs these. It’s not the first line of treatment, but it can be life-changing for the right patient.
8. Apicoectomy
This one sounds complicated but it’s actually quite targeted. An apicoectomy removes the very tip of a tooth’s root, along with any infected tissue around it.
It’s done when a standard root canal hasn’t fully resolved an infection. Instead of pulling the tooth, the surgeon goes in through the gum to address the problem at the root level. This saves the tooth.
9. Oral Cancer Biopsy and Tumor Removal
If your dentist spots a suspicious sore or growth in your mouth, they may refer you for a biopsy. A biopsy removes a small piece of tissue so it can be tested in a lab.
If oral cancer is confirmed, an oral surgeon plays a key role in removing the tumor. Early detection makes a significant difference in outcomes, which is one reason routine dental checkups are so important.
When Do You Need Oral Surgery?
Not every dental problem calls for surgery. But there are clear signs that point in that direction.
You might need oral surgery if you’re dealing with:
- Severe tooth decay that can’t be fixed with a filling or crown
- An impacted tooth that’s causing pain, swelling, or crowding
- Significant bone loss in your jaw
- Loose or missing teeth that need to be replaced
- A jaw that doesn’t align properly
- A persistent infection that hasn’t responded to antibiotics
- A suspicious lump or sore in your mouth that won’t heal
- Temporomandibular joint (TMJ) pain that’s affecting your daily life
Your dentist will usually spot these issues during a routine checkup or after looking at your X-rays. They’ll refer you to an oral surgeon when the situation goes beyond what they’re equipped to handle.
Don’t wait for pain to push you into action. Many of these conditions are easier to treat when caught early.
How to Prepare for Oral Surgery

Walking into any surgical procedure prepared makes everything smoother. Here’s what that typically looks like.
Your oral surgeon will start with a consultation. They’ll review your dental and medical history, take detailed X-rays or 3D scans, and explain exactly what the procedure involves. This is your chance to ask questions. Use it.
Depending on the type of anesthesia used, you may need to fast for several hours before the surgery. Your surgeon will give you specific instructions, follow them exactly.
Some medications can increase bleeding or interact with anesthesia. Tell your surgeon about everything you take, including vitamins and supplements. They’ll advise you on what to stop or continue.
Because sedation affects your reflexes and reaction time, you’ll need someone to drive you home. Plan for this ahead of time. You won’t be in a state to handle it yourself.
What to Expect During Oral Surgery
Walking into the procedure knowing what’s coming helps a lot.
Anesthesia Options
Your surgeon will discuss which type of anesthesia suits your procedure and comfort level.
- Local anesthesia numbs just the area being worked on. You’re awake but feel no pain.
- IV sedation keeps you relaxed and drowsy. You may not remember much of the procedure.
- General anesthesia puts you completely under. It’s typically reserved for longer or more complex surgeries.
How Long Does It Take?
That depends entirely on the procedure. A single tooth extraction might be done in 20 to 30 minutes. Corrective jaw surgery can take two to three hours. Your surgeon will give you a realistic estimate during your consultation.
Right After the Procedure
You’ll be moved to a recovery area. Staff will monitor you as the anesthesia wears off. You’ll receive clear instructions before you leave, covering medications, what to eat, and signs to watch for.
Oral Surgery Recovery: What to Expect
Recovery looks different depending on what was done. A simple extraction might have you back to normal in a few days. More involved surgeries can take weeks or even a few months for full healing.
The First 72 Hours
This is the most important window. Expect swelling, mild to moderate discomfort, and some bruising. Keep your head slightly elevated, even when sleeping. Apply an ice pack to the outside of your face for 15 to 20 minutes at a time during the first day.
Take your prescribed pain medication as directed. Don’t try to tough it out. Managing pain properly actually helps you heal better because you rest more comfortably.
What to Eat
Stick to soft foods for the first several days. Think yogurt, mashed potatoes, scrambled eggs, soups, and smoothies. Avoid anything hard, crunchy, or chewy. Stay away from hot liquids right after surgery because they can dissolve the blood clot forming at the surgical site.
That blood clot is important. Disturbing it leads to a painful condition called dry socket, which we’ll cover in a moment.
Keeping Your Mouth Clean
Oral hygiene during recovery is a bit of a balancing act. You need to keep your mouth clean but avoid disturbing the healing tissue.
Don’t rinse vigorously on the first day. From day two, gently rinse with warm salt water a few times daily. Brush carefully, avoiding the surgical area. Don’t use a straw, the suction can dislodge the clot.
And if you smoke, stop. Smoking is one of the biggest risk factors for complications after oral surgery. It slows healing and dramatically increases the chance of infection and dry socket.
Risks and Complications of Oral Surgery
Like any surgical procedure, oral surgery carries some risks. The good news is that serious complications are relatively rare, especially when performed by a qualified surgeon.
The most common issues to be aware of include:
Infection: Signs include fever, increased swelling after the first few days, pus, or a persistent bad taste in your mouth. People with diabetes or weakened immune systems are at higher risk. Antibiotics can usually clear this up.
Dry socket: This happens when the blood clot at the extraction site breaks down before the wound heals. It’s painful and slows recovery. Your surgeon can treat it by placing a medicated dressing in the socket.
Bleeding: Some bleeding is normal. If it doesn’t slow down after applying gentle pressure for 20 to 30 minutes, contact your surgeon.
Nerve effects: In rare cases, nerves near the surgical area can be bruised during the procedure. This may cause temporary numbness or tingling in the lips, chin, or tongue. Most nerve effects resolve on their own over weeks or months.
Adverse reaction to anesthesia: True allergic reactions are uncommon. Your surgeon will review your history to reduce this risk.
The skill and experience of your surgeon directly affects outcomes. Choosing someone who is board-certified and properly trained is one of the best ways to minimize risk.
Frequently Asked Questions
Is oral surgery painful?
During the procedure, you won’t feel pain because of the anesthesia. Afterward, discomfort is normal and manageable with medication. Most patients describe the pain as mild to moderate and say it’s much less scary than they expected.
How long does oral surgery take?
It varies. Simple extractions take 20 to 30 minutes. Dental implant placement can take an hour or more. Complex jaw surgeries may take two to three hours. Your surgeon will give you a clear estimate.
Does insurance cover oral surgery?
It depends on your plan and the procedure. Many dental insurance plans cover medically necessary oral surgeries, such as wisdom tooth removal or extractions. Cosmetic procedures typically are not covered. Always confirm with your insurance provider before your appointment.
Can I eat before oral surgery?
If you’re having local anesthesia only, you may be able to eat a light meal beforehand. But if sedation or general anesthesia is involved, your surgeon will likely ask you to fast for at least six to eight hours. Follow their specific instructions.
How long does recovery take after wisdom tooth removal?
Most people feel significantly better within three to five days. Full tissue healing takes about two weeks. The bone fully heals over several months, but you won’t notice that process happening.
What’s the difference between oral surgery and dental surgery?
They’re often used interchangeably. “Dental surgery” can refer to any surgical dental procedure, while “oral surgery” more specifically refers to the specialty performed by trained oral and maxillofacial surgeons. Think of oral surgery as a subset of dental surgery that covers more complex cases.
Final Thoughts
Oral surgery doesn’t have to be something you dread. Yes, the idea of a surgical procedure in your mouth sounds uncomfortable. But modern techniques, better anesthesia, and highly trained surgeons have made these procedures safer and more predictable than ever.
Whether you’re dealing with a stubborn wisdom tooth, a missing tooth that needs replacing, or a jaw issue that’s been affecting your quality of life, oral surgery often provides the kind of relief that nothing else can.
If your dentist has mentioned a referral, take it seriously. And if you have any doubts or questions, schedule a consultation. Getting clear information from a qualified surgeon is always the right first step.
Your oral health affects your overall health. Taking care of it is worth it.
Ready to take the next step? Consult with a board-certified oral surgeon in your area to discuss your specific situation and find the best path forward.