Gum infections affect millions worldwide, causing pain, swelling, and potential tooth loss if left untreated. Understanding the best antibiotics for gum infection is essential for effective treatment and preventing serious complications. This comprehensive guide explores proven antibiotic options, their mechanisms, and proper usage protocols.
Understanding Gum Infections and When Antibiotics Are Needed
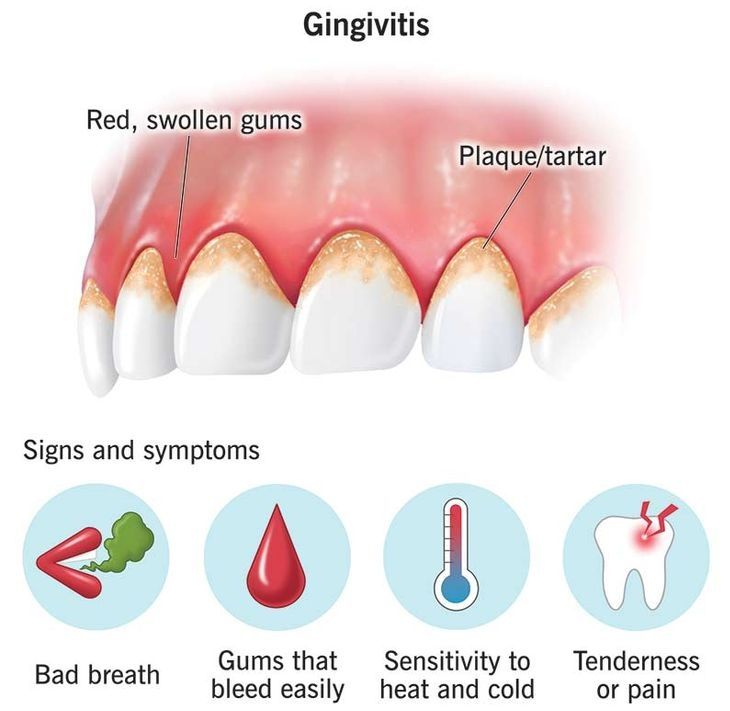
Gum infections, medically termed periodontal infections, occur when harmful bacteria accumulate beneath the gum line. These infections range from mild gingivitis to severe periodontitis, potentially spreading to surrounding bone and tissue. While professional dental cleaning forms the foundation of treatment, antibiotics become necessary when infections are severe, rapidly progressing, or accompanied by systemic symptoms like fever and swelling.
Dentists typically prescribe antibiotics for moderate to severe periodontitis, especially when deep gum pockets exceed 5 millimeters, aggressive bacterial growth threatens bone loss, or abscesses develop near tooth roots. Not every gum infection requires antibiotic intervention, many mild cases resolve through improved oral hygiene and professional cleaning alone.
Top 10 Best Antibiotics for Gum Infection
1. Amoxicillin
Amoxicillin ranks among the most commonly prescribed antibiotics for periodontal infections. This penicillin-type medication prevents bacteria from forming protective cell walls, effectively eliminating infection-causing organisms. The standard dosage is 500 mg three times daily for seven to ten days.
This broad-spectrum antibiotic targets various bacteria associated with gum disease, making it a reliable first-line treatment. When combined with clavulanic acid (sold as Augmentin), amoxicillin becomes resistant to bacterial enzymes that would otherwise inactivate it, expanding its effectiveness against resistant strains.
2. Metronidazole
Metronidazole specifically targets anaerobic bacteria thriving in oxygen-poor environments beneath the gums. Prescribed at 250-500 mg two to three times daily, this antibiotic inhibits bacterial DNA synthesis. Research shows metronidazole proves particularly effective for treating severe periodontitis, acute necrotizing ulcerative gingivitis, and chronic gum disease.
Dentists often combine metronidazole with amoxicillin for enhanced effectiveness against mixed bacterial infections. This combination therapy addresses both aerobic and anaerobic pathogens simultaneously, proving especially beneficial for aggressive periodontitis cases.
3. Doxycycline
Doxycycline offers unique dual-action benefits, both antibacterial and anti-inflammatory properties. This tetracycline-class antibiotic concentrates in gum tissue at levels 7-20 times higher than other medications. Beyond fighting bacteria, doxycycline inhibits collagenase, an enzyme that breaks down gum tissue and bone.
The typical dosage is 100 mg twice daily on the first day, followed by 100 mg once daily for 21 days. Low-dose doxycycline formulations (20 mg twice daily) are specifically designed for long-term periodontal disease management without contributing to antibiotic resistance.
4. Azithromycin
Azithromycin, a macrolide antibiotic, is known for reducing bacterial growth associated with periodontitis while providing anti-inflammatory benefits. This medication concentrates in neutrophils, macrophages, and fibroblasts, all critical cells in periodontal disease progression.
The standard regimen involves 500 mg on day one, followed by 250 mg daily for five days. Azithromycin proves particularly effective for smokers requiring reduced inflammation and patients who cannot tolerate other antibiotics. Its shorter treatment duration improves patient compliance significantly.
5. Clindamycin
For patients with penicillin allergies, clindamycin serves as an excellent alternative. This lincosamide antibiotic penetrates bone tissue effectively, making it ideal for severe gum infections spreading to the jawbone. Clindamycin stops bacterial protein synthesis, preventing growth and reproduction.
The typical dose is 300 mg four times daily. Clindamycin treats various serious bacterial infections and proves particularly useful for resistant cases or when other antibiotics fail to provide adequate results.
6. Ciprofloxacin
Ciprofloxacin, a fluoroquinolone antibiotic, targets gram-negative bacteria, including all strains of Aggregatibacter actinomycetemcomitans, a particularly harmful periodontal pathogen. This medication is currently the only antibiotic to which all A. actinomycetemcomitans strains remain susceptible.
Dentists prescribe ciprofloxacin for severe periodontal infections, especially when other antibiotics prove ineffective. It’s often combined with metronidazole for comprehensive coverage. The versatility of ciprofloxacin lies in its broad-spectrum activity against challenging bacterial strains.
7. Minocycline
Minocycline, another tetracycline derivative, is available in both oral and topical formulations. The topical version comes as microspheres (Arestin) placed directly into periodontal pockets during dental procedures. These tiny particles release medication gradually, providing sustained bacterial suppression.
Minocycline offers similar benefits to doxycycline, including antibacterial action and anti-inflammatory properties. The localized delivery system allows high antibiotic concentrations directly at infection sites while minimizing systemic exposure and potential side effects.
8. Penicillin V
Penicillin V represents a traditional antibiotic choice with proven ability to fight various oral bacteria. Despite being one of the oldest antibiotics, it remains prescribed for certain gum infections due to its effectiveness and affordability. However, some bacteria have developed resistance to penicillin V, potentially limiting its effectiveness.
Dentists may pair Penicillin V with other treatments or newer antibiotics for better results. Patients must complete the full course as prescribed and should skip this medication only if they have known penicillin allergies.
9. Cephalexin
Cephalexin, a first-generation cephalosporin, provides an alternative for patients with mild penicillin allergies. This beta-lactam antibiotic inhibits bacterial cell wall synthesis during active replication. The standard dosage is 500 mg four times daily for three to seven days.
While there’s approximately 10% cross-allergenicity between penicillins and cephalosporins, recent research shows cephalexin can be safely prescribed for many penicillin-allergic patients under proper medical supervision. It effectively treats various gram-positive bacteria associated with periodontal infections.
10. Erythromycin
Erythromycin, a macrolide antibiotic, demonstrates bacteriostatic activity against bacteria causing dental infections, particularly Streptococcus mutans. This antibiotic inactivates bacterial growth and decreases dental plaque formation. The typical dosage ranges from 250 to 500 mg every six hours.
However, erythromycin isn’t regularly recommended due to potential gastrointestinal problems, hepatotoxicity risks, and bacterial resistance development. It’s contraindicated in patients taking certain medications or suffering from specific conditions, requiring careful medical evaluation before prescription.
Topical Antibiotic Treatments
Beyond oral medications, dental professionals utilize topical antibiotic applications, including Atridox (doxycycline gel), PerioChip (chlorhexidine chips), and Arestin (minocycline microspheres). These localized treatments deliver high antibiotic concentrations directly to infected areas while minimizing systemic exposure and side effects.
How Antibiotics Work Against Gum Disease
The best antibiotics for gum infection function through various mechanisms, some prevent bacterial cell wall formation while others inhibit protein or DNA synthesis. Certain antibiotics like doxycycline provide anti-inflammatory benefits beyond antimicrobial action. They break down bacterial defenses, stop reproduction, and allow the immune system to heal damaged tissue.
Proper Antibiotic Usage and Compliance
Complete the entire prescription, even when symptoms improve early. Stopping prematurely can lead to resistance and recurrence. Common side effects include digestive upset and nausea. Contact your dentist immediately for severe reactions like difficulty breathing, severe rash, or persistent diarrhea.
Combining Antibiotics with Professional Treatment
Antibiotics work best alongside professional dental interventions. Scaling and root planing remove plaque and tartar below the gum line that antibiotics alone cannot eliminate. Improved oral hygiene, including brushing, flossing, and antimicrobial mouthwash, helps prevent reinfection.
Antibiotic Resistance and Responsible Use

Overuse of antibiotics contributes to bacterial resistance. Dentists carefully evaluate necessity and select appropriate options based on specific bacteria and patient history. Never use leftover antibiotics or medications prescribed to others, only dental professionals can determine the best antibiotics for gum infection based on individual circumstances.
Special Considerations for Different Patients
Specific populations require special consideration: pregnant or breastfeeding women should avoid tetracyclines, patients with penicillin allergies need alternatives like clindamycin or azithromycin, and individuals with liver or kidney disease may require modified protocols.
Prevention: The Best Strategy
While antibiotics treat active infections effectively, prevention remains optimal. Maintaining excellent oral hygiene, quitting smoking, managing diabetes, and addressing teeth grinding significantly reduce infection risk. Some patients explore natural antimicrobial agents like salt water rinses as supplementary treatments, though these should never replace professional care or prescribed antibiotics.
When to Seek Immediate Dental Care
Seek urgent dental attention for persistent gum pain, severe swelling, pus discharge, fever, difficulty swallowing or breathing, or rapidly progressing symptoms. Untreated gum infections can lead to tooth loss, bone damage, and systemic complications.
FAQs
What antibiotic kills gum infections?
Amoxicillin (500mg, three times daily) is the first-line antibiotic for gum infections, effectively killing bacteria causing periodontal disease. Metronidazole (500mg, twice daily) targets anaerobic bacteria in severe cases. For penicillin allergies, dentists prescribe clindamycin or azithromycin. Always complete the 7-10 day course as directed by your dental professional.
How do you treat swollen gums in children?
Rinse with warm salt water (½ teaspoon per cup) twice daily to reduce inflammation. Ensure proper brushing with soft-bristled toothbrush and age-appropriate fluoride toothpaste. Apply cold compress externally for 10 minutes to ease discomfort. Avoid sugary foods and maintain hydration. If swelling persists beyond 48 hours, fever develops, or pain worsens, consult a pediatric dentist, untreated gingivitis can progress to serious infections.
How to get rid of a tooth abscess while pregnant?
See a dentist immediately, tooth abscesses during pregnancy require professional treatment to prevent complications affecting mother and baby. Your dentist may perform drainage or root canal therapy, which are safe during pregnancy. Penicillin-based antibiotics like amoxicillin are pregnancy-safe (Category B). Rinse with warm salt water for temporary relief. Avoid aspirin and ibuprofen; use acetaminophen (Tylenol) for pain. The second trimester is ideal for dental procedures, but emergencies need immediate care.
Can a tooth infection cause shoulder pain?
Yes, a tooth infection can cause referred shoulder pain, particularly from upper molars. Infected teeth share nerve pathways (trigeminal and cervical nerves) with neck and shoulder regions, causing radiating pain. Lower tooth infections may refer pain to the jaw and shoulder blade. If you experience shoulder pain with toothache, facial swelling, fever, or difficulty swallowing, seek immediate dental care, this indicates spreading infection requiring antibiotics and possibly emergency extraction or root canal treatment.
Conclusion
The best antibiotics for gum infection serve as powerful tools in dental care when used appropriately under professional guidance. From amoxicillin and metronidazole to specialized options like ciprofloxacin and azithromycin, each antibiotic offers unique benefits for specific situations.
Success requires combining proper antibiotic therapy with professional dental cleaning, improved oral hygiene, and regular checkups. Only qualified dental professionals can determine the most appropriate antibiotic based on individual patient needs, ensuring optimal oral health outcomes while minimizing antibiotic resistance risks.
Remember, antibiotics complement, not replace, comprehensive periodontal treatment. Working closely with your dentist and following prescribed treatment plans provides the foundation for healthy gums and a lasting smile.